Most of the time, claw and hammer toe are deformities of one or more of the four lesser toes. The affected toe is bent over itself, its joints flexed downwards.
There are three major types of toe deformities of this kind, namely: the hammer toe, claw toe and mallet toe. Their difference is the location of the flexed joint: for hammer toes, the affected joint is the farthest to the toenail. On the contrary, mallet toe corresponds to the flexion of the joint closest to the toenail. Lastly, the claw toe is flexed at both joints.
When to have surgery for hammer toes?
Hammer toe surgery is the last-line treatment approach and only planned if medical treatments have been insufficient. These first treatments include orthopaedic insoles to correct, if necessary, imbalance in the distribution of loads at the forefoot, which is responsible for the deformity.
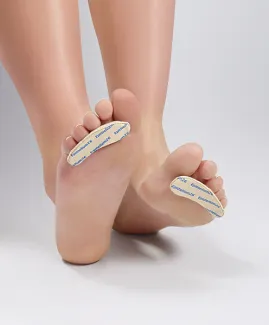
Also, toe orthotics or toe straighteners like the hammer toe cushions* directly address the deformity. This device smoothly lies down the four lesser toes. In addition, some exercises are recommended by physical therapists and podiatrists to improve symptoms of hammer toes.
What are the common techniques of hammer toe surgery?
On the one hand, the choice of the surgical technique for hammer toe surgery depends on toe mobility. Indeed, either the deformity can be corrected (the joint is still movable), or it can’t be (the joint is no longer movable). On the other hand, the technique is chosen according to the cause of onset of the problem.
Let’s remember that hammer toes can come from altered pressure at the forefoot (flat foot, hollow foot or bunion for example). It can also be due to a tendon contracture caused by muscle imbalance. Before surgery, the surgeon identifies whether the problem is related to bones, tendons, or both.
Techniques of surgery for tendons
- Tenotomy
For claw toes, tendon contracture sometimes is the origin of the deformity. These tendons pass under the toes and, if they’re contracted, they impede the toe to lie flat on the ground. To face this problem, the main action is to cut the tendon, which is called ‘tenotomy’. This technique is mainly used for still flexible toes(2).
- Tendon lengthening
That is the objective of stretching exercises made with the physical therapist. This time, the procedure is surgical and allows to increase the length of the tendon in order to correct the contracture.
- Tendon transfer
Tendon transfer is a type of surgery that consists of modifying the function of a muscle. It is possible by changing the insertion point of the muscle’s tendon.
Techniques targeting bones and joints
- Osteotomy
Osteotomy is used to cut a bone, here the phalanx of the affected toe in order to shorten it. This surgery usually addresses the first phalanx of the toe(4).
- Arthroplasty
Surgical reconstruction of a stiff joint to re-establish its mobility is named arthroplasty. Often, hammer toe surgery focuses on the proximal interphalangeal joint and consists of removing the head of the phalanx(3, 5).
- Arthrodesis
Surgical fusion of a joint, or arthrodesis, is used for advanced cases, when the joint is stiffened(2). For hammer toes, the fusion usually concerns the proximal interphalangeal joint(3). This type of hammer toe surgery does not systematically require pins or implants which will be removed once the joint has fused.
- Arthrolysis
Arthrolysis is a surgical procedure that loosens an ankylosed joint, when movements are limited. To do so, the surgeon cuts the retracted tissues (joint capsules or membranes that link bone surfaces within a joint). This approach commonly focuses on the metatarsophalangeal joint or proximal interphalangeal joint(3, 4).
The four surgical procedures are the most common for claw and hammer toe surgery. Also note that in most cases, the surgeon uses several techniques to correct the deformity of hammer toes(3).
Hammer toe surgery: before/after
The objective of hammer toe surgery
The main aim of hammer toe surgery is pain relief. Indeed, some shoes put pressure on the prominent joint and cause the formation of painful corns on the top of the toe.
The second objective is to avoid the deformity to worsen and its insidious consequences. Hammer toe progressively induces excessive loads at some weight-bearing areas of the forefoot, especially under the metatarsal heads(2). This leads to the formation of calluses.
Lastly, the hammer toe should be definitively straightened. It prevents discomfort in the shoe and aesthetic problems. Hammer toe surgery aims to re-establish contact between the pulp of the toes and the ground(1).
What to expect during surgery?
Hammer toe surgery is normally made on an outpatient basis: the patient arrives and goes back home the same day of surgery. However, the duration of surgery varies whether the hammer toe is associated with another deformity like hallux valgus or bunion.
Usually, this surgery just requires local anaesthesia (only the foot). Two main procedures exist: the open surgery or the percutaneous (micro-incisions) surgery.
Recovery
After hammer toe surgery, the surgeon applies a compression bandage that should not be removed until the next follow-up appointment.
Just after surgery, you can walk or drive on condition that you wear a special off-loading shoe. You should also limit weight bearing for your foot and elevate your legs regularly to reduce foot swelling.
A few days after surgery, you could start rehabilitation exercises with a physical therapist(3).
Are there complications of such surgery?
Hammer toe surgery is riskier according to the age, lifestyle and potential comorbidities. For example, people with diabetes should be particularly watched(1).
There are some post-surgical complications which are common to any surgery: haematoma, oedema, wound healing problems or infections.
There are also more specific complications to hammer toe surgery. They include hypo- or hypercorrection of the deformity, problems of bone consolidation and risks of recurrence.
The diversity of deformities, their causes, surgical techniques and all the criteria to take into account make hammer toe surgery complicated. For more details about mallet, claw or hammer toe surgery, click here and seek advice from your general practitioner or podiatrist.
*This solution is a class I medical device that bears the CE marking under this regulation. Carefully read the instructions before use. Manufacturer: Millet Innovation. 12/2023
For more details about this general and simplified approach, here are further sources:
(1)Diebold P-F. Pathologie non traumatique des orteils. EMC - Appareil locomoteur. janv 2009;4(3):1‑6.
(2)Bissuel T, Canovas F, Avignon A, Sultan A. La chirurgie orthopédique dans la prévention des troubles trophiques du pied chez le patient diabétique. Médecine des Maladies Métaboliques. févr 2016;10(1):47‑52.
(3)Etchevers J-P. Ténodèse des fléchisseurs par l’implant Toe-Flex® dans le traitement des griffes d’orteils. Med Chir Pied. juin 2016;32(2):51‑3.
(4)Frey S, Hélix-Giordanino M, Piclet-Legré B. Correction percutanée de la déformation proximale du 2e orteil par arthrolyse de l’interphalangienne proximale, ténotomie du Flexor Digitorum Brevis et ostéotomie de la phalange proximale. Revue de Chirurgie Orthopédique et Traumatologique. oct 2015;101(6):498‑503.
(5)Société d’Imagerie Musculo-Squelettique. Le pied [Internet]. Sauramps Médical; 2011 [cité 12 avr 2022]. Disponible sur: http://www.sims-asso.org/uploads/pdfs/monographies/3/1.pdf
 Pharmacie
Pharmacie