You think you have a bunion on your foot? How to diagnose a bunion? Whom to consult to establish bunion diagnosis? EPITACT® gives you answers!
If your first symptoms suggest that you have a bunion or hallux valgus, do not wait any longer to consult a specialist. Some specific tests can be realised to identify a bunion and its stage of development.

How to identify a bunion?
The bunion diagnosis is often obvious, although it has differential diagnoses. There are three major steps to be sure you suffer from a bunion: clinical and podoscope examination and bunion x ray. Now, discover how to recognise a bunion step by step.
Do not try to make a self-diagnosis. Although the Web is a large source of information, your case is unique! Only a health professional is able to establish the proper diagnosis taking into account every symptom and their history.
First step for the bunion diagnosis: the non-weight-bearing examination
The diagnosis for bunions starts with a clinical examination which is performed by a health professional. At first, the physician practices a visual exam. He examines the medial bony bump (the bunion) and measures the angles of the deviation. The first angle corresponds to the deviation between the big toe and the first metatarsal bone. The second angle is the one between the first and the second metatarsals.
Then, he can ask you some questions to collect information about your medical and family history, symptoms…
He can also manipulate the foot, especially the toes, to assess the mobility of the joints and the structure of your feet. The clinical exam also includes a range of motion tests for the metatarsophalangeal joint (MTP).
At the same time, he observes the skin to detect possible cutaneous affections (of the skin) such as calluses or corns. He can also see if there is an inflammation called bursitis which often occurs when the toes rub and press the shoe repeatedly.
How to recognise a bunion with a podoscope examination?
To diagnose a bunion, the doctor can do a podoscope examination. It allows him to see below the feet while you’re standing and bearing your whole weight. The aim is to distinguish the areas of excessive support but also the deformities when the feet are in a weight-bearing position.
This exam assesses the severity of the valgus position once the feet is weight-bearing but also overload on certain areas (e.g.: insufficiency of the first ray and weight transfer on the second one for example). It also leads to the analysis of potential compensatory behaviours (fallen arch, deformities of the rearfoot, torsion between the front and the rear of the foot, retraction of the Achilles tendon). These few examples and a disorder of the ankle mobility can have negative consequences on the superior parts of the body like the knee or the hip.
Indeed, the interest of the static and dynamic examination is to assess the reasons for consultation considering that the foot is just the final functional element forming the lower limb. Assessing the patient as a whole is crucial.
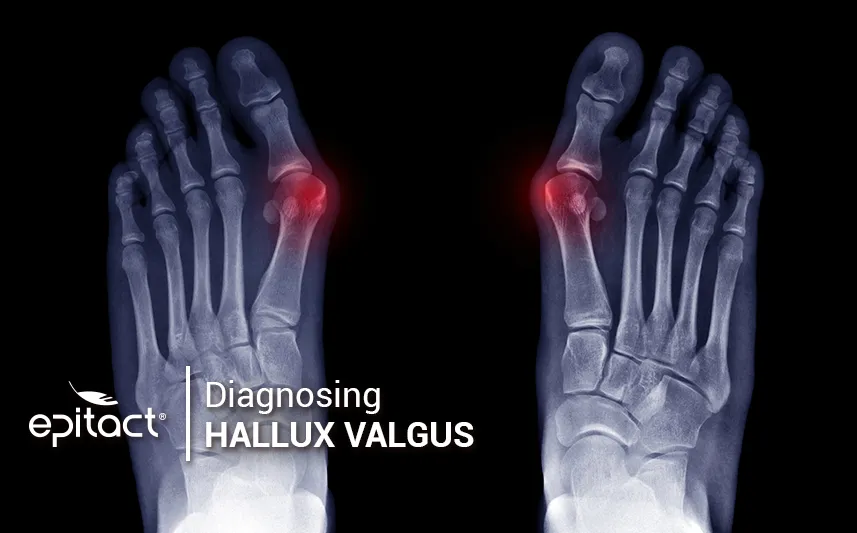
How to diagnose a bunion with X-Ray imaging?
A radiological assessment aims to confirm the pre-diagnosis of hallux valgus. Il analyses precisely the angles of deviation. Thanks to this, the doctor has all the necessary information to consider which curative or corrective options could be possible.
In addition, bunion X-rays show the consequences of the hallux deviation on its neighbouring toes but also on the whole structure of the foot. An X-ray of both feet from the top allows one to observe the deformity angle. Moreover, an X-ray is to be taken of both feet on the dorsal-plantar surface (from the top), weight-bearing and in schuss, i.e. with the knees flexed at 30°.
Lastly, two further images are required: one barefoot, in profile and weight-bearing, the other to observe the sesamoid bones (from the front, weight-bearing, also called the Guntz view).
Who can diagnose a bunion hallux valgus?
If you have a bunion, you should consult your general practitioner. He is the one who makes your consultation part of the healthcare system and diagnoses your bunion. He also plans a regular follow-up and monitors the progression of the deformity to assess your symptoms. In addition, when it is necessary, he can advise you to see a foot specialist. Your podiatrist helps you choose the best treatment for you. You can also see an orthopaedist, especially if you have a severe hallux valgus. He can recommend you to undergo surgery as the treatment of last resort.
What to do if you have a bunion?
First, wear shoes with a wide toe box and avoid high-heeled and poor-fitting shoes. According to the severity of the condition, changing of habits and correcting the deformity with a specific device can be recommended.
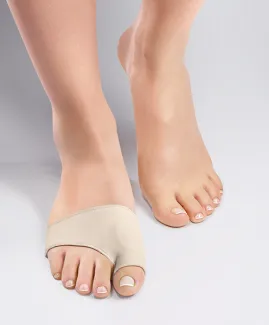
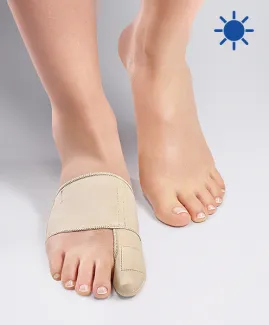
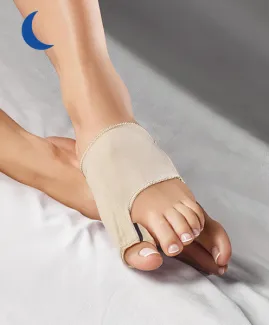
If you have a mild bunion but which causes you pain when walking, try the EPITACT®flexible bunion corrector*. At night, wear the rigid bunion corrector* that relieves you while it realigns your big toe. If you have a severe bunion, you can prevent bunion pain. EPITACT® has created a bunion protector* that reduces the friction and pressure on the big toe joint from the shoes. Remember that hallux valgus is a deformity that cannot disappear over time.
So If these former nonsurgical treatments are insufficient, a more invasive option will be the only alternative: surgery. Because each case is unique, the practitioner is the only one able to choose the proper treatment, provided that you agree with this invasive option.
Now you know how to diagnose a bunion and whom to consult to identify it. For further information, discover how a bunion forms and how to stay sexy with hallux valgus. Also, find out the preventive and corrective measures that you can preemptively adopt to reduce your pain and deformity.
*These solutions are class I medical devices that bear the CE marking under this regulation. Carefully read the instructions before use. Manufacturer: Millet Innovation. 07/2021
 Pharmacie
Pharmacie