When it comes to treat a bunion, correction surgery is the treatment of last resort. It is usually recommended for severe bunions, also called hallux valgus.
This article doesn’t detail all the surgical techniques used to treat a bunion but only the most frequent ones. In 1952, McBride already counted more than 50 techniques, whereas nowadays, there are over 180!
If there are as many techniques, it is mainly for the purpose of being able to provide a solution for all the different cases. By the way, it is rare to perform only one technique to correct bunions. A global approach is usually preferred and includes several complementary techniques in order to adapt to the patient situation. With EPITACT®, discover the major techniques for bunion correction surgery.
How to correct bunions?
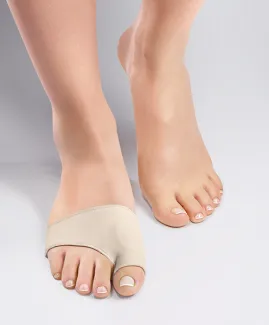
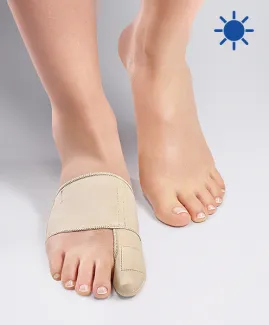
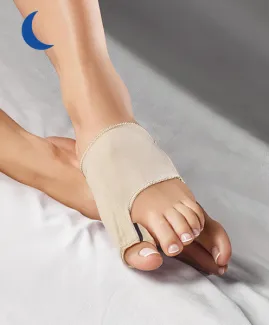
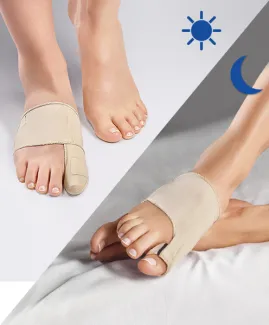
There are different ways of realigning the big toe, but the only permanent one is surgery. You can also correct the deviation by using specific devices: bunion correctors or toe spacers for example. However, both types of products help to straighten the big toe and limit the symptoms of hallux valgus but do not avoid its progression or lasting realignment.
However, the EPITACT® day and night bunion correctors have proven to be effective: 79% and 92% of patients observed a realignment of their big toe after 1 month, respectively(1, 2).
Many factors influence the type of surgery for the correction of hallux valgus
The choice of performing surgery to treat a bunion or the type of procedure depend on many factors:
- foot architecture;
- age and gender of the patient;
- severity of the condition;
- speed and type of progression;
- potential reluctance of the patient;
- patient capacity to adapt his/her behaviour (shoes habits, weight...);
- intensity and ambitions linked with sports activity;
- risks entailed and the potential complications specific to each case;
- season (spring/summer favour the recovery after surgery due to the possibility of wearing open-toe or light shoes).
Main techniques for the bunion correction surgery
There are two types of correction surgeries for bunions which can be combined:
• The first one targets the soft parts (tendons, ligaments) and aims to correct a moderate deformity in the metatarsophalangeal joint;
• The second one concerns the bones:
o The cutting of a bone (osteotomy) allows to modify the axis of the bone;
o The fixation of two parts of a bone (osteosynthesis) by screws, pins or staples is the most frequent technique.
Generally, several techniques are performed during one surgical procedure to correct this complex and local deformity called hallux valgus.
Metatarsophalangeal arthrolysis of the big toe
This surgery is often part of a set of complementary processes realised during one surgery. Cutting or lengthening of the joint capsule and peripheral ligaments allow a correction of the big toe joint deformity.
McBride procedure
This surgery combines a bunionectomy (bone abrasion) with the cutting of the adductor hallucis tendon at the base of the phalanx. Before, it was also combined with the removal of the lateral sesamoid bone. Cutting the tendon stops its aggravating effect on the valgus deviation of the toe; the transfer of this tendon on the head of the first metatarsal then contributes to correcting the metatarsus varus.
Nowadays, bunion correction surgery is almost no longer used. Indeed, removing the lateral sesamoid frequently resulted in the unforeseen varus deviation of the hallux, that is to say in the opposite direction. Because the toe is deviated outwards, it becomes extremely complicated to wear shoes.
Simple abrasion of the exostosis
Bunionectomy means bunion removal but it does not correct the misalignment. It involves the abrasion of the medial part of the metatarsal head (the prominent part of the bone is sawed or milled) that reduces the medial bony protrusion and makes the wearing of shoes easier. However, since the hallux has not returned to its normal axis, the deformity will continue its progression.
Proximal phalangeal osteotomy of the big toe
This bunion correction surgery is based on a double V-shape cut (chevron osteotomy) or the use of a rotary burr to remove a part of the bone in the medial base, then allowing to correct the valgus deviation of the hallux. This part removed can be trapezoidal, thicker on the inner side (medial).
It allows shortening of the big toe when it is necessary according to the patient’s morphotype (‘Egyptian foot’). A fixation (osteosynthesis) can be realised, either temporarily with a pin (metal rod removed after bone consolidation) or definitively with a screw or staple.
Chevron distal metatarsal osteotomy
A V-shaped cut (chevron) of the first metatarsal neck corrects the metatarsus varus. This technique can often be used during a minimally invasive-percutaneous surgery to correct bunions. The incision, which is only a few millimetres long, soothes pain and facilitates recovery. A fixation with a pin or staple can be necessary.
Scarf osteotomy of the first metatarsal
The term scarf comes from the vocabulary of carpentry ‘hook scarf” which is a Z-shaped cut that allows joining two pieces of wood together. The scarf procedure is one of the most common osteotomies to treat hallux valgus.
In this bunion surgery, a Z-shaped cut of the first metatarsal bone is performed in the horizontal plane with an oscillating micro-saw. Its inferior and distal part is moved towards the other toes (up to 50% of its width), which corrects the varus deformity. An osteosynthesis with 2 vertical screws is often realised. This procedure is usually performed by open surgery.
Wide and flexible shoes with thick soles are recommended for the postoperative period. Then, weight-bearing walking rehabilitation is necessary depending on the pain experienced. Two to three months bunion correction surgery, resuming physical activities normally and wearing normal shoes can be considered.
Arthrodesis of the first metatarsophalangeal joint
This technique for the correction of hallux valgus consists of fusing the proximal phalanx of the big toe with the first metatarsal after removing the cartilaginous articular surfaces of these two bones. Bone fixation (osteosynthesis) with screws or a screw plate is the most often required.
It is especially used for the treatment of hallux rigidus but rarely for hallux valgus.
Implant arthroplasty of the first metatarsophalangeal joint
In some cases, using a prosthesis to keep the mobility of the joint is an alternative. Several types of prostheses exist for diverse functions (resurfacing implant of the phalanx or metatarsal bone, or interposition implant).
This kind of surgical procedure is extremely rare to correct a bunion.
None of these bunion correction surgeries is exempt from risks of complications, even weeks after surgery. Your surgeon will tell you about those risks and how to make sure it heals properly.
It remains crucial to wear shoes that fit one’s morphology and to wear adapted silicone protections to prevent and relieve bunion pain. In this way, EPITACT® offers a wide range of bunion pads to daily protect the forefoot* or bunion correctors to realign the big toe during the day* or at night*.
Actually, bunion correction surgery treats the double deviation associated with hallux valgus, but without real change of habits, recurrence is possible. Hallux valgus is a deformity that cannot disappear over time. EPITACT® gives you some practical advice to shrink bunions naturally.
*These solutions are class I medical devices that bear the CE marking under this regulation. Carefully read the instructions before use. Manufacturer: Millet Innovation. 09/2021
Sources:
(1)Clinical evaluation conducted by Podyconcept in May 2011 on 39 patients with hallux valgus.
(2)Clinical evaluation conducted by Podyconcept in July 2015 on 15 patients with hallux valgus.
 Pharmacie
Pharmacie